Overview
We break down the payment infrastructure stack into 4 main layers. We anchor with payment rails at the bottom because the nuance of provider's cash flows and how payers think about float on claims they are paying out impacts money movement across this stack.
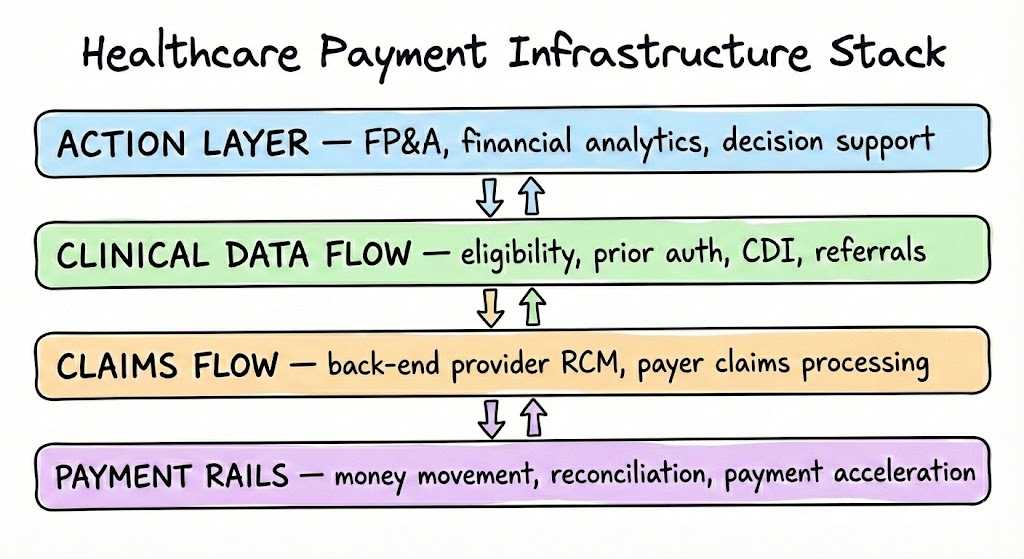
The unifying thesis across these layers is that there's an opportunity to drive payer rules to the point of care. Today, most of the intelligence in this stack runs after the fact. Claims get submitted, edited, denied, appealed, then paid 60 days later on rails that separate the money (EFT) from the explanation (ERA), requiring manual reconciliation. The structural shift is that every layer is moving from batch/post-hoc to real-time/pre-bill.
Payment Rails. ERAs (remittance data) and EFTs (money) travel on separate rails. Payers batch hundreds of claims per transmission and payment and remittance don't arrive together and are constrained by 80-character ACH limits that strip context. The cash flow pain is severe enough that we've seen providers who will accept a 50% take-rate on accelerating performance-based revenue just to get paid now instead of waiting 18 months. The opportunity we see here is payment acceleration to predict what a claim will pay, advance the funds, and reconcile when adjudication catches up.
Claims Flow. The status quo today is mostly post-pay but this is shifting as both providers and payers are now automating this cycle in a much discussed AI arms race. The structural shift is that the intelligence is moving pre-pay. On the payer side, pre-pay payment integrity grew from virtually nonexistent a decade ago to 40%+ today, trending toward 60%+ over the next 2-3 years. The opportunity we see here is pre-pay payment integrity for the companies that can flag errors and FWA before adjudication can capture the highest-ROI position in the claims flow.
Clinical Data Flow. We have worked with companies on the pre-bill CDI side purely focused on providers (e.g., SmarterDx). We see a continued shift here where tools similar to Optum Real (but payer-agnostic) push payer rules to the point of care to validate claims in real time. Providers adopt these solutions because of reduced admin costs as payers provide these tools for free or low-cost, and can get paid faster. Payers are pushing these tools to reduce admin costs on their end (prior auth, claims editing, payment integrity) but the ROI has to be above and beyond the float they make on these delayed claim payouts today (45+ days AR typically).
Action Layer. Today, CFO teams spend weeks manually crosswalking Excel files to find margin leakage and underpayment against contractual terms. Up to 5% of net revenue is missed through underpayment that providers can't currently detect at scale. The shift isn't better reporting but automating the next best action. AI-native FP&A tools (e.g., Translucent) don't just surface underpayment in seconds on live data but they trigger the appeal, flag the contract term, and route the action to the right person. The opportunity is turning financial intelligence into automated decisions rather than dashboards.
What This Means Going Forward
The opportunity is in the seams between layers. The question for founders is which wedge, not whether the tools are good enough to build more performant solutions than incumbents. Each layer has a proven entry point: second-pass claims editing on the payer side (prove ROI on dollars Cotiviti missed, then migrate to first-pass), workflow-specific or specialty-specific RCM automation on the provider side (own one vertical like infusion or spine before going horizontal), reconciliation automation on payment rails (additive layer, no rip-and-replace), etc. In each case, the wedge works because you don't need to displace an incumbent to start generating value.
The insurer margin crisis creates buyer urgency that didn't exist two years ago. UNH's MCR climbed to 89.25%, Elevance's MLR hit 91.26% (up 175bps), and industry margins are at their lowest point in two decades. Every basis point of MLR improvement is worth $10B+ to the industry. UNH is targeting $1B in AI-enabled cost reductions for 2026 but 95% of claims already auto-process, meaning the easy gains are taken. The next wave of savings requires infrastructure modernization across the stack, not incremental optimization of existing tools.
Additional Reading
Elevance Lower Revenue/Membership 2026
CMS Flat 2027 MA Rate Proposal
Machinify Acquires Performant ($670M)
